Industry
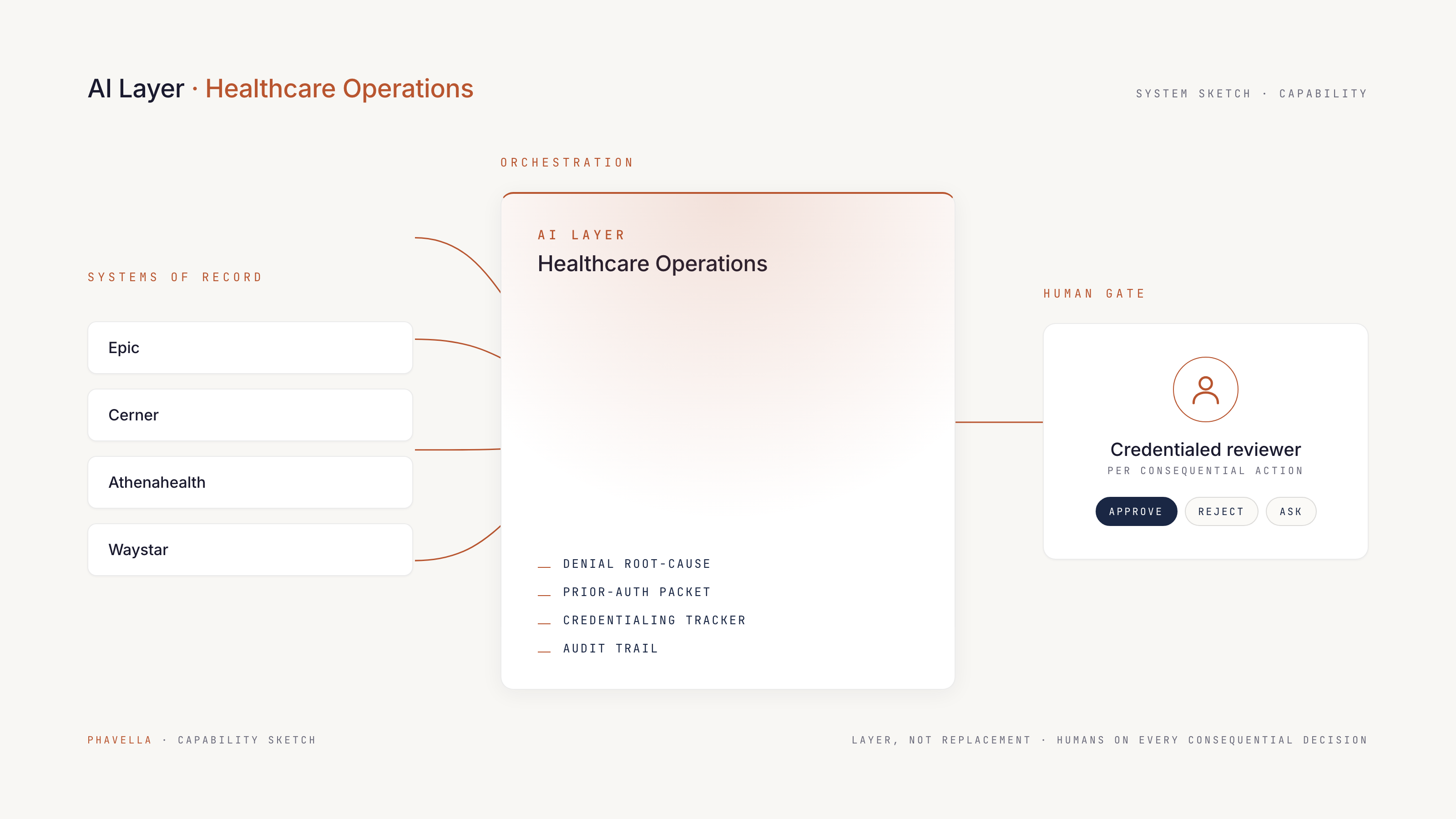
Healthcare Operations
Back-office and revenue-cycle workflows for healthcare operations, never clinical, always with a credentialed reviewer in the loop.
What the work usually looks like.
A multi-site provider, lab network, or specialty group running on Epic / Cerner / Athena plus a billing platform and a tangle of payer portals. Revenue cycle leaks. Credentialing takes months. Operations leaders manage a workforce against PHI rules that limit what AI can see directly.
Where we tend to find the constraint.
- Denials that age out because the billing team never reaches the appeal
- Credentialing files that go silent for weeks at a time
- Schedule gaps that nobody notices until the day before
What we typically build for operations like yours.
Claim denial root-cause and appeals drafting (with credentialed reviewer sign-off)
Prior-auth packet assembly from EHR + supporting records
Credentialing-document tracking and renewal prompts
Schedule-fill optimization with site-manager approval
Vendor / payer contract performance monitoring
Where the human gate goes, specifically for this industry.
Healthcare ops is where HITL is non-negotiable. We do not propose autonomous clinical decisions, period. Back-office workflows route every consequential action through the credentialed person responsible for it, and PHI exposure is contained at the system boundary.
Talk to us
Have an operation in this shape?
We'll start with a 2-week Discovery against your real systems. If we're not a fit we'll say so on the call and point you somewhere useful.